|
 
- 现金
- 62111 元
- 精华
- 26
- 帖子
- 30441
- 注册时间
- 2009-10-5
- 最后登录
- 2022-12-28

|
本帖最后由 StephenW 于 2011-5-25 23:02 编辑
http://www.medscape.com/viewarticle/715052
Occult Hepatitis B Virus Infection: A Covert Operation
Introduction
A 2008 international workshop on occult hepatitis B virus (HBV) infection (OBI), endorsed by the European Association for the Study of the Liver (EASL),[1] defined OBI as the 'presence of HBV DNA in the liver (with detectable or undetectable HBV DNA in the serum) of individuals testing hepatitis B surface antigen (HBsAg) negative by currently available assays'. The definition implies that infectious viral clones may be present. However, the detection of HBV DNA does not always correspond to infectivity or to the number of HBV progeny viruses released from hepatocytes. Therefore, unless infectivity has been established, clinicians should be careful in their use of terms such as OBI or occult hepatitis B viremia in deference to the more comprehensive term 'occult hepatitis B (OHB)'.
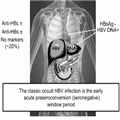
About 20% of OHB sera are negative for all serological markers of HBV infection except HBV DNA, 50% are positive for hepatitis B core antibody (±anti-HBs), and 35% are positive for hepatitis B surface antibody (±anti-HBc)[2] (Fig. 1). On the basis of these HBV antibody profiles, OHB may be further stratified into seropositive or seronegative categories with the seronegative subjects being negative for both anti-HBc and anti-HBs. The HBV DNA levels are lowest in these subjects. Seropositive individuals can be further divided into two groups: anti-HBc positive, with or without anti-HBs. The HBV DNA detection rate is highest in subjects who are anti-HBc positive but anti-HBs negative, and these individuals are more likely to be infectious. When present, HBV DNA levels are intermediate in anti-HBc– and anti-HBs–positive persons. The quintessential occult HBV infection occurs in the early acute pre-seroconversion (seronegative) window period prior to the detection of HBsAg. However, OHB also may be observed in anti-HBc positive patients with chronic HBV infection following the decline of HBsAg to an undetectable level that is sometimes associated with the appearance of anti-HBs. This serological pattern occurs at a rate of 0.7–1.3% per year and is associated with older ages and hepatitis B e antibody (anti-HBe) reactivity.[3–7]
 (Enlarge Image) (Enlarge Image)
| Figure 1. Consensus definition of occult hepatitis B.
|
In the last decade, the application of highly sensitive molecular biology techniques has led to greater recognition and diagnosis of OHB and elucidation of its virological and clinical features. This clinical entity has been reported in healthy blood donors, patients with chronic liver disease and in patients with hepatocellular carcinoma. However, several aspects of OHB are still not resolved including the clinical significance of OBI as it relates to the risk of transmission, reactivation and progression to chronic liver disease.
Molecular and Immunopathogenetic Mechanisms Associated with Occult Hepatitis B
The molecular basis of OHB is linked to the peculiar life cycle of HBV. A key step in replication of the virus is conversion of the 3.2 -kb circular DNA into a covalently closed circular DNA (cccDNA) in the nucleus of infected hepatocytes. The cccDNA is the template for transcription leading to production of new virions. This highly stable cccDNA is resistant to enzymatic digestion or to current antiviral agents and is the basis for persistence of HBV infection. The median cccDNA copies/hepatocyte is estimated to be approximately 1.5, but ranges from <0.01 to >50 copies/cell.[8] These levels strongly correlate with intracellular and serum HBV DNA and are lowest in patients with occult hepatitis B.[9]
It is estimated that an average-sized liver contains approximately 2 × 1011 hepatocytes and that 5–40% of these hepatocytes are infected at any given time.[10] Virions are assembled and released from the cell at a rate of 1–10 HBV particles/day for a total daily expression of 1010–1012 particles. Concurrently, from 103 to 105 noninfectious, subviral HBsAg particles are being released each day in excess of the virus.[11] The finding of cccDNA, RNA transcripts and pregenomic replicative RNA intermediates in the liver, peripheral blood mononuclear cells (PBMC) and/or blood of a large proportion of infected patients suggests that most occult infections are caused by low-level replication of wild-type virus.[12,13]
The reasons for persistence of low levels of HBV DNA in the absence of detectable HBsAg remain largely undefined, but it is conjectured that both host and viral factors are important in suppressing viral replication and keeping the infection under control.[14–17] Zerbini et al.[18] studied HBV-specific T-cell responses in patients with OHB, with or without anti-HBc, and identified two different profiles. Anti-HBc–positive patients showed a T-cell response typical of protective memory suggesting that this condition represents a resolved infection with immune-mediated virus control. In contrast, an HBV-specific T-cell response was not seen in anti-HBc–negative patients, suggesting the possibility that a low-level viral infection may be insufficient to allow maturation of protective memory. These results suggest different mechanisms of control of viral replication in seropositive and seronegative OHB patients.
In addition to these host responses, low levels of viral replicative activity may result from the presence of defective interfering particles or to mutations in transcription control regions or the polymerase domain leading to inefficient replication in conjunction with the discordant release of HBsAg by the hepatocytes.[17,19,20] Repression of viral transcription by cytokines induced during HBV clearance suppresses replication resulting in HBsAg negativity and low or undetectable levels of serum HBV DNA in the presence of intrahepatic HBV DNA. It also has been observed that HBsAg polypeptides are important in regulating the release of HBV and noninfectious 20-nm subviral particles from the hepatocyte. In this process, a high level of the L or large protein of HBsAg, a virion envelope component, enhances HBV morphogenesis and secretion from the hepatocyte and downregulates release of noninfectious HBsAg particles. Conversely, low levels of the L polypeptide regulate the recycling of HBV DNA-containing nucleocapsids to the nucleus and enhance the release of subviral particles from the cell. At the same time, high levels of the S or small polypeptide of HBsAg promote assembly and secretion of excess quantities of noninfectious HBsAg particles from the cell independent of virion release.
Additional mechanisms responsible for HBsAg negativity in OHB include (i) binding of HBsAg to anti-HBs to form immune complexes;[21] (ii) the development of mutations affecting the 'a' epitope of the S gene that encodes amino acid residues within the major hydrophilic loop of the HBsAg coding region rendering the virus and its noninfectious particles nondetectable by current HBsAg assays; or (iii) coinfection with hepatitis delta virus or hepatitis C virus (HCV) that results in downregulation of HBV replication and a reduction in antigen synthesis.[22] This inverse correlation between the concentration of HCV RNA and HBV DNA is shown in Fig. 2.[23] Correspondingly, in transfused recipients concurrently infected with HBV and HCV, the initial appearance of HBsAg is often delayed followed by a shortened interval of HBsAg detection, a reduction in peak HBV DNA concentration and a lower peak alanine aminotransferase (ALT) level when the HBsAg first becomes positive compared to transfusion-associated HBV monoinfections[url=][24][/url] (Fig. 3). Previously, it was shown that HCV core protein inhibits HBV replication and gene expression,[25] but this observation has recently been challenged by Bellecave et al.[26] who observed that HBV and HCV can replicate in the same cell line without evidence for direct interference in vitro. Therefore, the HBV viral interference observed in coinfected patients is probably a result of indirect mechanisms mediated by innate and/or adaptive host immune responses.[24,27]
==================================================
The reasons for persistence of low levels of HBV DNA in the absence of detectable HBsAg remain largely undefined, but it is conjectured that both host and viral factors are important in suppressing viral replication and keeping the infection under control.
因此比较良性???(except in HCV and alcohol cirrhosis patients)
|
|